Supervised by: Amanda Liu, BEng, MSc. Amanda spent her undergraduate years studying Biochemical Engineering at UCL (University College London), where she was awarded First Class Honours. She then completed her Master’s degree in Clinical and Therapeutic Neuroscience at the University of Oxford. She is currently studying Medicine (Graduate Entry) at the University of Cambridge.
Throughout all time, humans have kept pace with different enemies, both natural and artificial, visible and invisible. Today, the world is in an arduous fight against the Coronavirus. ‘We are in the Wild West.’, said one COVID patient (1). Here, ‘We’ simultaneously refers to COVID patients, healthcare workers, and the general public. Without a doubt, every single person is involved in the battle against the coronavirus. While the virus has brought a colossal death toll, its scope for mental health influence is even more substantial. ‘What does this mean for my family and me?’; ‘What if I bring germs home with me?’ (2). Alongside the virus, anxiety, depression, post-traumatic stress disorder (PTSD) and more have also spread across the globe, particularly among youngsters, who have less experience coping with traumatic crises (3). This paper will spotlight the impact of mental health on adolescents, particularly the social, economic, and personal implications.
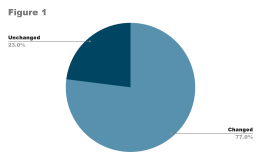
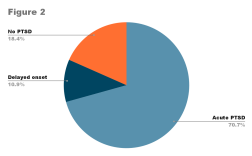
While social wellbeing is one of the three cornerstones of mental health (4), social relationships are hindered by the various social restrictions imposed by governments due to COVID. The problem is exacerbated by the characteristics of teenagers, who rapidly develop interactions outside their home and frequently have high energy levels (5, 6). Using quarantine as an example, the experience of being deliberately isolated for a period of time can seem tedious, frustrating and confusing for us all, with clear indications that a disconnection with the world can develop in this period (7). According to a study in Italy and Spain, 77% of parents have reported a change in the emotional state and behaviour of their children (8, fig.1). Moreover, from the previous experience in the Asian earthquake and subsequent tsunami of 2004 (9 fig.2), the Fukushima nuclear accident (10), and other disasters, it is possible to project that a substantial portion of youth will develop PTSD in the future. Many claim that the use of social media is a way of avoiding this, but it may be too optimistic to suggest social media cures the problem without evaluating the potential additional harm it can bring.
Some critics consider social media as ‘especially pernicious’ when it comes to the spread of information, since many users are ‘driven not by facts but by emotion, bias, prejudice, and lies’ (11). For instance, the myth that vaccination has links to autism (12) contributes to negative perceptions of vaccination, helplessness and hopelessness amongst parents and an unpleasant environment online (11, 13). What makes the problem worse is the illusory truth effect, which is the tendency of people to believe information that is repeatedly mentioned; social media algorithms tend to prioritise information that one has come across before, creating something of an echo chamber (14). In addition, the tendency of people to fill in knowledge gaps, often through speculation or inaccurate musing on social media (11), exacerbates the harm. A famous experiment of a man promoting his shed to a top-ranked restaurant on a popular website through deception shows that the potential effect of social media is gigantic (15) – much more substantial than the ordinary person’s expectation. Although social media can improve the connection between family and friends in times of isolation, it very clearly has flaws.
Besides the social shock, the economic challenge posed by the pandemic across the globe is also worth consideration. Primarily resulting from limitations on local trading and a plunge in consumer confidence, the UK faces its most significant economic crisis in 300 years (16). Subsequently, many have lost jobs and, by extension, their incomes (17). This leads, in turn, to a decline in mental health, indicated by a drastic increase in suicidal and alcohol abuse rates (18, 19). A considerable proportion of people believe that finance is a matter that only adults consider, but this is not true. According to research conducted in Sweden, a negative correlation between the percentage of adolescents caught in psychosomatic problems and financial affairs has been revealed (20). External factors, both social and economic, can precipitate a decline in adolescents’ mental health. However, these factors do not guarantee a decline in mental health, suggesting that the ways in which these external factors are interpreted can lead to the damage of their mental health, rather than the factors themselves.
Although awareness of the pandemic is appropriate, it is not rational when worrying is disproportionate to the risk. One fundamental factor that exaggerates the harm is catastrophic thinking, which is a tendency to imagine the worst possible outcome. According to an investigation, teenagers are amongst the most likely groups to exhibit catastrophic thinking (21), contributing to a sense of being ‘out of control’. This could go some way to explaining the 6.3% rate of clinical anxiety in Norwegian adolescents (22). Some professionals suggest that having a high emotional awareness can cure the problem by conscious prevention (23), and indeed the younger population tends to be better in this area, yet a substantial portion is lagging behind (24). Health organizations encourage individuals to seek help from doctors when they are concerned about their mental health (25), especially when they fail to recover locally. Still, it is questionable whether accessing this care is feasible in times of COVID.
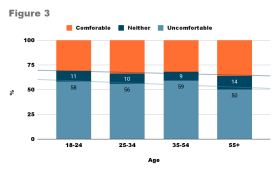
Often, the most effective phobia treatments constitute both psychotherapy and medication. Psychotherapy stems from developing confidence to face the source of the phobia via repeated exposure (26), which can seem to sacrifice patient safety and wellbeing. This is unlikely to be an appropriate treatment for the distress caused by COVID-19, leaving weakened treatment options, with only medication and alternative therapies available. Seeking external help could be further complicated by the stigma persisting around mental health. From an investigation in the US, only approximately one-third of the population is comfortable discussing their mental illness, even with their family and friends (24, fig.3). Although only adults are included in this study, all age groups report a similar figure and additional studies suggest that teenagers are reluctant to seek help, and most adolescents’ mental health conditions remain undetected (25, 26, 27).
In contrast to physical health, mental health is more of a subtle concept. As can be seen from the arguments above, adolescents’ mental health problems from COVID will be tough to handle, with a range of social, economic, and personal implications.
However, as ‘there is no health without mental health’ (28), governments should take measures to diversify support options available to adolescents, and offer ways to improve their mental health status if needed. For instance, providing forums tailored for teenagers enables them to express their emotions online and discover people in a similar situation. Still, details of this are beyond the scope of this paper.
Comment
This research paper uses a variety of online resources and the majority of them are selected from reputable individuals or organisations. However, there are some limitations including: 1. A limited scope of sources are used (only from western countries), therefore they may not be representative in the world’s scope, and 2. Some assumptions are made (as mentioned in the main body), which may have a significant impact on the accuracy of this passage.
Bibliography
Vos, J. (2021) The Psychology of Covid-19: Building Resilience for Future Pandemics. 1st edn. SAGE Publications. Available at: https://www.perlego.com/book/2094729/the-psychology-of-covid19-building resilience-for-future-pandemics-pdf (Accessed: 16 August 2021).
COVID-19 and Mental Health. www.youtube.com, https://www.youtube.com/watch?v=CVvGvoMRUhk. Accessed 16 Aug. 2021.
‘BBC World Service – The Evidence, Coronavirus: The Evidence, Mental Health and the Pandemic’. BBC, https://www.bbc.co.uk/programmes/w3ct2czw. Accessed 16 Aug. 2021.
What Is Mental Health? | MentalHealth.Gov. https://www.mentalhealth.gov/basics/what-is-mental-health. Accessed 16 Aug. 2021.
kontakt.zones.sk, (c) Tím Zones sk-Najväčší študentstký portál –. ‘Characteristics of young people’. Zones.sk, https://www.zones.sk/studentske-prace/anglictina/19620- characteristics-of-young-people/. Accessed 16 Aug. 2021.
Post-COVID Syndrome: Mental Health. www.youtube.com, https://www.youtube.com/watch?v=Rn306wjvl3g. Accessed 16 Aug. 2021. 7. ‘BBC World Service – The Evidence, Coronavirus: The Evidence, Mental Health and the Pandemic’. BBC, https://www.bbc.co.uk/programmes/w3ct2czw. Accessed 16 Aug. 2021.
Imran N, Aamer I, Sharif MI, Bodla ZH, Naveed S. Psychological burden of quarantine in children and adolescents: A rapid systematic review and proposed solutions. Pak J Med Sci. 2020;36(5):1106-1116. doi: https://doi.org/10.12669/pjms.36.5.3088
‘BBC World Service – Health Check, Mental Health and the Long Term Implications of Covid’. BBC, https://www.bbc.co.uk/programmes/w3ct1nv1. Accessed 16 Aug. 2021.
‘BBC World Service – Health Check, Mental Health and the Long Term Implications of Covid’. BBC, https://www.bbc.co.uk/programmes/w3ct1nv1. Accessed 16 Aug. 2021.
Kelly, B. (2020) Coping with Coronavirus: How to Stay Calm and Protect your Mental Health. 1st edn. Irish Academic Press. Available at: https://www.perlego.com/book/1414893/coping-with-coronavirus-how-to-stay-calm and-protect-your-mental-health-pdf (Accessed: 16 August 2021).
Gerber, Jeffrey S., and Paul A. Offit. ‘Vaccines and Autism: A Tale of Shifting Hypotheses’. Clinical Infectious Diseases : An Official Publication of the Infectious Diseases Society of America, vol. 48, no. 4, Feb. 2009, pp. 456–61. PubMed Central, https://doi.org/10.1086/596476.
‘How Do Thoughts and Emotions Affect Health?’ Taking Charge of Your Health & Wellbeing, https://www.takingcharge.csh.umn.edu/how-do-thoughts-and-emotions affect-health. Accessed 16 Aug. 2021.
‘COVID and False Beliefs: How Social Media Exploits Cognitive Bias’. Medscape, http://www.medscape.com/viewarticle/950367. Accessed 16 Aug. 2021.
I Made My Shed the Top-Rated Restaurant on TripAdvisor. https://www.vice.com/en/article/434gqw/i-made-my-shed-the-top-rated-restaurant-on tripadvisor. Accessed 16 Aug. 2021.
StackPath. https://www.instituteforgovernment.org.uk/sites/default/files/publications/cost-of covid19.pdf. Accessed 16 Aug. 2021.
Panchal, Nirmita, et al. ‘The Implications of COVID-19 for Mental Health and Substance Use’. KFF, 10 Feb. 2021, https://www.kff.org/coronavirus-covid-19/issue brief/the-implications-of-covid-19-for-mental-health-and-substance-use/.
de Goeij, Moniek C. M., et al. ‘How Economic Crises Affect Alcohol Consumption and Alcohol-Related Health Problems: A Realist Systematic Review’. Social Science & Medicine (1982), vol. 131, Apr. 2015, pp. 131–46. PubMed, https://doi.org/10.1016/j.socscimed.2015.02.025.
Barr, Ben, et al. ‘Suicides Associated with the 2008-10 Economic Recession in England: Time Trend Analysis’. BMJ, vol. 345, Aug. 2012, p. e5142. www.bmj.com, https://doi.org/10.1136/bmj.e5142.
Kim, Yunhwan, and Curt Hagquist. ‘Trends in Adolescent Mental Health during Economic Upturns and Downturns: A Multilevel Analysis of Swedish Data 1988- 2008’. J Epidemiol Community Health, vol. 72, no. 2, Feb. 2018, pp. 101–08. jech.bmj.com, https://doi.org/10.1136/jech-2017-209784.
Bollen, James. ‘What Is Catastrophising?’ CPD Online College, 14 June 2021, https://cpdonline.co.uk/knowledge-base/mental-health/what-is-catastrophising/.
Hafstad, Gertrud Sofie, et al. ‘Adolescents’ Symptoms of Anxiety and Depression before and during the Covid-19 Outbreak – A Prospective Population-Based Study of Teenagers in Norway’. The Lancet Regional Health – Europe, vol. 5, June 2021. www.thelancet.com, https://doi.org/10.1016/j.lanepe.2021.100093.
Dodgson, Lindsay. ‘Constantly Imagining the Worst Case Scenario Is Called “catastrophising” — Here’s How to Stop Your Mind from Doing It’. Business Insider, https://www.businessinsider.com/what-catastrophising-means-and-how-to-stop-it 2018-3. Accessed 16 Aug. 2021.
Aware. https://www.mentalhelp.net/aware/the-stigma-of-mental-illness/. Accessed 16 Aug. 2021.
Radez, Jerica, et al. ‘Why Do Children and Adolescents (Not) Seek and Access Professional Help for Their Mental Health Problems? A Systematic Review of Quantitative and Qualitative Studies’. European Child & Adolescent Psychiatry, vol. 30, no. 2, Feb. 2021, pp. 183–211. Springer Link, https://doi.org/10.1007/s00787- 019-01469-4.
Adolescent Mental Health. https://www.who.int/news-room/factsheets/detail/adolescent-mental-health. Accessed 16 Aug. 2021.
‘Children and Young People’. Mental Health Foundation, 7 Aug. 2015, https://www.mentalhealth.org.uk/a-to-z/c/children-and-young-people.
Mental Health: Strengthening Our Response. https://www.who.int/news-room/fact sheets/detail/mental-health-strengthening-our-response. Accessed 16 Aug. 2021.




