Supervised by: Faissal Sharif BSc, MSc, DPhil cand. (Oxon). Faissal obtained a BSc in Biomedical Sciences at Maastricht University with a semester abroad at the Chinese University of Hong Kong. As a visiting scholar at the University of California, Irvine, he investigated biomarkers for Alzheimer’s Disease. He completed his MSc in Translational Neuroscience at Imperial College London. Beyond his work on psychiatric disorders and mental health, Faissal has developed an interest in the connection between medicine and technology through working with Medtech and Digital Therapeutic startups and organizations such as the European Space Agency. Currently, he is completing his DPhil at Oxford University in Clinical Neuroscience, focusing on novel neurotechnology to fight mental disorders.
ABSTRACT
Addiction causes individuals to repeatedly take or do something that will eventually be harmful to themselves. Addictions can develop towards drugs, gambling, alcohol, etc. Addiction is a pressing issue in society as it can affect many. It may begin by affecting the brain chemistry, changing how chemicals associated with pleasure such as dopamine are released during the engagement in an addictive behaviour. There are multiple theories on addiction that provide an explanation as to how certain drugs and behaviours lead to dependency in individuals. The addiction cycle and incentive-sensitisation theories are examples of such theories. The addiction cycle refers to the idea that tolerances are built up after using specific substances that create a euphoric or pleasant feeling after usage. The three stages explained in this paper are: binge/intoxication, withdrawal/negative affect phase, and finally the preoccupation/anticipation stage. The second theory, incentive-sensitisation theory, proposes the idea that drug addiction involves the individual to “want” the substance. This “wanting” has been overamplified by the brain and triggers cues of craving the substance/behaviour without amplifying “liking”.
This paper addresses four types of addiction; alcohol addiction, heroin and cocaine addiction, social media addiction, and sugar addiction. The diverse selection of additives allows readers to learn about different types of substance addictions, in addition to reading about behavioural addictions as well. Alcohol, heroin and cocaine addiction are examples of substance addictions in which the body produces pleasurable feelings during use and causes a dependency on these substances when the substance exits the system. Addictions such as sugar and social media addiction, occur similarly but the brain is stimulated by the behaviour. Therefore, it requires repetition of the behaviour to continue the feelings of pleasure or enjoyment.
Some current therapies for addiction include drug therapy, Naltrexone (for alcohol addiction), Methadone, Nicotine Replacement Therapy, behavioural therapy and psychotherapy. Drug therapies can help reduce withdrawal symptoms when substances are stopped. Naltrexone is used to treat alcohol and opioid addiction which reduces the pleasurable feelings of alcohol or opioids. Methadone is an opioid that reduces withdrawal symptoms and cravings. Nicotine Replacement Therapy is used for nicotine addiction to ease people off of nicotine in products like gum, patches and inhalers. Finally, behavioural therapy and psychotherapy are used for behavioural addictions using the behavioural patterns and causes of the individual to tackle the root problem. Some future therapies that are under scientific study include “psychedelics” such as mushrooms that cause reduced craving. Another future therapy includes electric current therapy for non-invasive brain stimulation to reduce addictive behaviour.
INTRODUCTION
Addiction is the inability to control doing, taking, or using something to the point where it could be harmful to an individual. It is typically associated with the use of substances, however it is possible to be addicted to a variety of behaviours including work, internet, shopping, etc. (NHS, 2021).
Addictive substance use refers to patterns of symptoms resulting from its use, despite experiencing negative mental and physical effects as a result. Induced disorders refer to intoxication and withdrawal induced mental disorders (Hartney, 2022).
Substance-related disorders were specifically acknowledged in ten different types of drugs in the chapter “Substance-Related and Addictive Disorders” within the The Diagnostic and Statistical Manual of Mental Disorders V (DSM-V). Only gambling disorders are classified as a behavioural addiction in the section of “non-substance-related disorder” in the DSM-V, but the majority of behavioural addictions were not identified as such (Hasin et al., 2013).
Addictions are not to be confused with dependency. Dependency disorders are characterised by the presence of withdrawal symptoms—physical manifestations that arise when an individual ceases the use of the substance they’re dependent on. Addiction, on the other hand, is defined by an uncontrollable need to consume or interact with a particular substance or activity, often at the expense of daily functions and responsibilities. Both conditions can lead to detrimental long-term consequences, including neuroadaptation—a term denoting enduring changes in brain structure and function due to sustained substance misuse. There are primarily four categories of drugs: stimulants, opiates, depressants, and hallucinogens. Among these, alcohol, classified as a depressant, ranks as one of the most widely abused substances globally.
Addiction also affects overall public health, from alcohol addiction to substance misuse disorders. In a recent study, more than 27 million people in the United States reported uses of illicit drugs or misuses of prescription drugs, and nearly 25% of adults and adolescents reported binge drinking in the past month (Assistance Secretary for Health, 2023). The consequences of drug abuse affect not only individuals but also their families, businesses, and government resources.
When dealing with addiction, two neurological pathways come into play. First, the mesolimbic dopamine reward pathway. Necessary for survival, this pathway can undergo changes due to substance use, resulting in overwhelming cravings. Abnormalities in the mesolimbic pathway can also affect the likelihood of developing an addiction. Second, drug abuse can modify the prefrontal cortex responsible for decision-making – a region that inhibits inappropriate reward responses (Clay, 2008). Even though studies have shown that it is possible to control drug addiction through pharmacological and cognitive-behavioural therapy (Liu & Li, 2018), such interventions for Substance Use Disorder (SUD) and Alcohol Use Disorder (AUD) often have a high relapse rate, especially in the first weeks. Relapse can occur due to stress, reward system stimulation, or even by a singular dose of the addictive substance (Clay, Allen & Parran, 2008). It is estimated that 40% – 60% of individuals treated for SUD relapse, posing a medical challenge and an opportunity for research of alternative methods (National Institute on Drug Abuse, 2020).
This review aims to assess the various theories, types and treatments of addiction in order to provide insight into future directions.
THEORIES OF ADDICTION
The Addiction Cycle
A person may develop a tolerance after using a substance when it is consumed to feel euphoric or fulfilled. The cycle of addiction is the term used to describe the process of becoming addicted.
There are three key phases to this process: the binge/intoxication phase, the withdrawal/negative affect phase, and the preoccupation/anticipation phase. The stages specifically involve three domains: executive function, negative affective states, and incentive salience. The extended amygdala, prefrontal cortex, and basal ganglia are the three major areas of the brain where each of the three domains is located (National Institute on Drug Abuse, 2020).
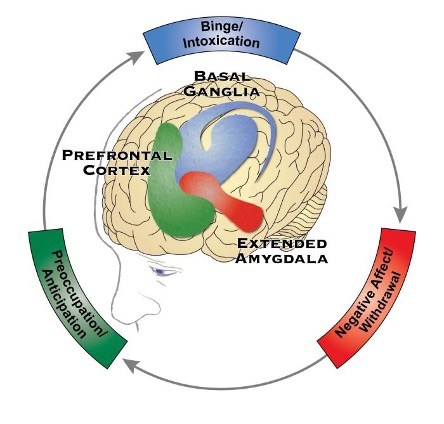
Figure 1: National Institute on Alcohol Abuse and Alcoholism, 2021
Stage 1: Binge/Intoxication
After the intake of an “addictive” substance, the binge and intoxication stage occurs when a person feels certain rewarding benefits, such as anxiety relief, and a sense of happiness. This stage takes place in the basal ganglia, a part of the brain that contains the caudate nucleus, putamen, and globus pallidus. It is also in charge of a person’s involuntary behaviours, such as tremors (Cleveland Clinic, 2022).
When people take “addictive” substances, the dopamine pathway in the basal ganglia may be activated, causing a strong rush of pleasure. People may try to consume more of the substance because the dopamine system is stimulated by the rush of pleasure. As a result, people are triggered to use more drugs to achieve the same pleasure (National Institute on Drug Abuse, 2020).
Stage 2: Withdrawal/Negative Affect Phase
The negative affect phase, or the withdrawal stage, involves the amygdala and occurs when a person discontinues their addiction and starts to experience withdrawal symptoms. This includes physical symptoms such as pain and sleep disturbances as well as emotional symptoms, such as dysphoria, anxiety, and irritability (National Institute on Alcohol Abuse and Alcoholism, 2021). Such symptoms may vary in terms of intensity and duration depending on the type of substance used and severity of use. At this stage, a decreased activation in the reward systems of the basal ganglia, or less dopamine, obstructs the person’s ability to experience pleasure. This is followed by an increased activation of the brain’s stress systems, which includes stress neurotransmitters such as norepinephrine in the extended amygdala (SurgeonGeneral, 2016).
Stage 3: Preoccupation / Anticipation
In the preoccupation/anticipation stage of addiction, a person experiences cravings after a period of abstinence. Although these cravings do not directly link with relapse, the person may become preoccupied with, or look forward to, using the addictive matter again (National Institute on Alcohol Abuse and Alcoholism, 2021). This stage happens in the brain’s prefrontal cortex, which plays a vital role in thought organisation, planning, and decision making. This causes a disruption to dopamine and glutamate regulation and impairs the person’s emotional control and decision making, causing cravings. The lack of decision-making ability becomes a motivator to engage in risky behaviour to pursue more of the addictive behaviour. People with addiction are unable to cut out their addictions even with attempts and desires to do so (Genesis Recovery, n.d.).
Incentive-Sensitization Theory
According to the Incentive-Sensitization Theory, drug addiction is a psychological “wanting” that has been overly amplified and is triggered by cues, without necessarily amplifying “liking” (Berridge & Robinson, 2016). The two physically and neurochemically separate brain systems that govern ‘wanting’ and ‘liking’ typically cooperate to impact motivation, but they may become dissociated in the process of someone becoming addicted (Warlow et al., 2020).
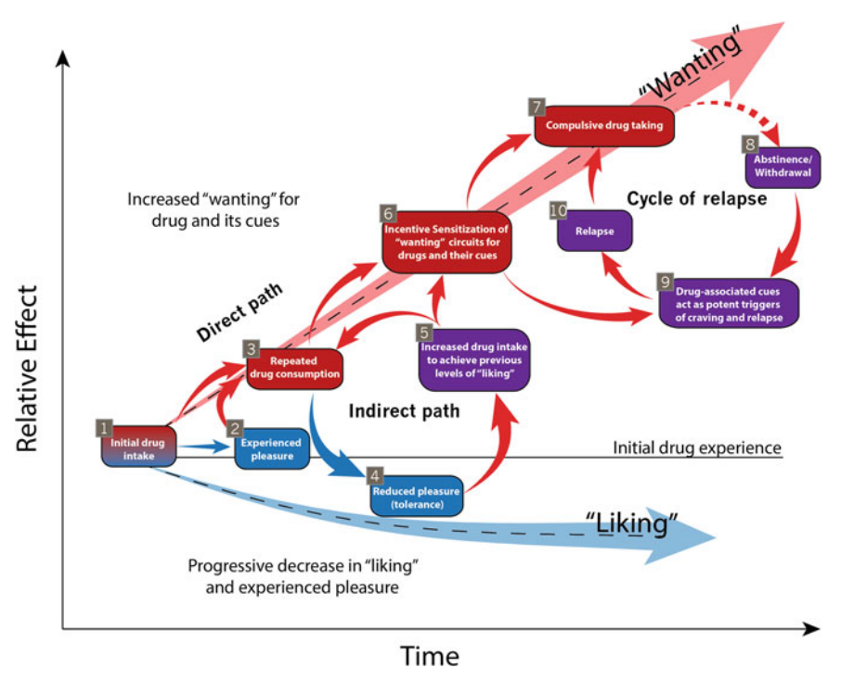
Figure 2: Robinson et al., 2015
An addictive drug is a stimulus that activates the mesolimbic pathway and sets off neurobiological events that influence that system. The intensified “wanting” for drugs is not matched by an intensification of “liking” for the same drugs. Dissociation occurs because, even for the same reward, brain “liking” and “wanting” systems can function somewhat independently of one another. The “wanting” might increase independently of whether a drug is still “liked” after several uses because only “wanting” systems become sensitised (Poland & Graham, 2011).
In contrast to the “wanting” system, the smaller functional system called “liking” produces intense levels of pleasure. The “liking” system includes a collection of interactive hedonic hotspots which is a circulatory system that shares diverse pleasurable feelings. For example, sensory food, drug pleasures, and social pleasures (Berridge & Kringelbach, 2015).
The pleasure-generating hotspots are physiologically small, resulting in the reason for intense pleasures being uncommon. Hedonic hotspots exist in the prefrontal cortex where they may correspond to sensory codes and high pleasures. Others can be “buried” deeper into the brain structure. The role of dopamine seems to be restricted to “wanting” as dopamine stimulations, by contrast, always fail to enhance “liking” (K.C Berridge & Kringelbach, 2015; K.S. Smith et al., 2011).
For normal capacities of pleasure there may be hedonic hotspots found in the ventral pallidum which is located at the base of the subcortical forebrain (K.S. Smith & Berridge, 2007). Furthermore, the ventral pallidal hotspot is the only site known to eliminate normal pleasure by reversing the impact of a stimulus from “liked” to “disliked”.
Addiction itself distorts “wanting” and “liking”. When using drugs of abuse, this system is stimulated when the drugs are taken repeatedly, at large doses across periods of time. This causes mesolimbic sensitisation and can change other neurotransmitters and neurons and physical structures of mesolimbic neurons. In conclusion, addicts have stronger urges and intense “wanting”. However, “liking” doesn’t increase with sensitisation and may decrease.
TYPES OF ADDICTIONS
Alcohol
Alcoholism is one of the most common addictions in the world. Alcohol addiction manifests itself in many ways, including the volume/amount of alcohol consumed as well as the frequency of drinking. The main alcohol addiction symptoms include a high tolerance to alcohol, no or little hangover symptoms, increased volume consumed, depression/anxiety, consistent thoughts of consumption, and drinking during inappropriate scenarios (for example, at work or in the morning, etc.). Alcohol can create a feeling of giddiness and ecstasy as intoxicated people experience emotions stronger than those who are sober. However, it can also create symptoms such as nausea, slurred speech, vomiting, aggression, confusion, unconsciousness, and can get to a state where they are unable to coordinate their movement. Ethanol is the primary chemical in alcohol which brings about these effects commonly associated with alcohol consumption. When the brain’s chemical balance is off-balanced by ethanol, the typical effects of alcohol are experienced due to impaired brain function as they affect each lobe. Many studies have shown that ethanol is targeting gamma-aminobutyric acid (GABA). GABA is the main inhibitory neurotransmitter in the Central Nervous System (CNS). GABA-A are receptors that decrease the excitability in neurons, which ethanol binds to. GABA-A intervenes with the excitatory neurotransmitter (glutamate), which is responsible for carrying signals between nerve cells in the body. Glutamate’s ability to communicate is inhibited due to the ethanol (Promises Behavioral Health, 2017). The ethanol in alcohol can create many issues if overused for long periods of time.
Alcoholism can also lead to a variety of illnesses, syndromes and diseases. For example, Wernicke Korsakoff syndrome, in which the major cause is alcoholism. The main symptoms including mental confusion, changes to the eyes and vision, and memory issues are due to the complex and delicate brain chemistry that becomes severely affected by the alcohol consumed. It occurs due to a vitamin B1 (thiamine) deficiency (Healthline, 2012). This therefore impairs processes such as the utilisation of carbohydrates into energy for the body, and affects all vital organs, especially the brain. The main areas of the brain that become affected include the cerebellum, brain stem, hypothalamus and cerebral bodies. Due to the excess consumption of alcohol, and depending on the sufferer’s post-diagnosis choices, it can become irreversible brain damage.
As well as a psychological dependence, alcohol can also produce physical addiction. Heavy drinking over a long period can create dependency. If the drinker attempts to stop suddenly, they may experience sweating, shaking, severe depression, nausea, and may go into shock or die (Alcohol Change UK, 2020). In England, there are an estimated 602,391 dependent drinkers, and the global average consumption was 6.1826344 litres per person (Alcohol Change UK, 2020; Ritchie & Roser, 2018).
Heroin and Cocaine
An opioid is a substance which binds to opioid receptors in the central nervous system; these can be endogenous, semi-synthetic, or synthetic, and are classed as depressants (Seminars in Perinatology, 2019). Endogenous opioids are important in pain relief, inducing euphoria, and controlling food intake (Biochemistry, Endogenous Opioids, 2022).
Heroin is an example of a semi-synthetic opioid. Its desired effect is euphoria, however there are many negative effects such as insomnia, liver and kidney issues, abscesses, and difficulty with concentration. Cocaine is not classed as an opioid, and is a stimulant which acts as a dopamine reuptake inhibitor. This means that it increases mood by allowing more dopamine to be absorbed over time in the brain. Symptoms include paranoia, alertness, anxiety, and happiness. The cause of death for heavy cocaine users is heart issues such as cardiotoxicity or heart attacks, however, since opioids are depressants, they typically slow down the nervous system and cause death by inducing respiratory depression, as is the case for heroin (Banyan Treatment Centers, 2023). According to SAMHSA, in 2018 approximately 10.3 million people abused prescription opioids and heroin in the USA, and 2.2 million people abused cocaine.
Social Media
Addiction can occur in many forms. Unlike alcohol and drug abuse, social media is a form of a behavioural addiction. As the term implies, behavioural addiction refers to the compulsion to repeatedly engage in an activity regardless of the negative impact on the person’s ability to remain mentally and/or physically healthy (American Addiction Centres, 2019). Multiple studies have found a strong link between heavy social media and an increased risk for depression, anxiety, loneliness, self-harm, and even suicidal thoughts (Robinson & Smith, 2023). Social media has become an addiction for more than 210 million people, with 40% being aged between 18 to 22 years old. Despite the fact that social media allows consumers to express themselves and communicate with their peers, it possesses the capability to do more harm than good. As a result of social media distractions, disruption of sleep, bullying, rumour spreading, peer-pressure, and unrealistic views of other people’s lives, researchers have shown that social media addiction can affect mood, cognition, physical, emotional, and interpersonal problems, as well as psychological problems (Hou et al., 2019). Additionally, adolescents are highly sensitive to acceptance and rejection through social media. Their heightened emotional sensitivity and protracted development of reflective processing and cognitive control make them specifically reactive to emotion-arousing media (Crone & Konijn, 2018). Adolescents may be more susceptible to harmful comments on social media due to this, resulting in a reduction in confidence and creativity. Therefore, social media can be highly addictive and can have numerous effects detrimental to one’s physical and mental health.
Sugar
Often, food for which individuals experience cravings is either sugary, salty, fatty, or all three. Unlike food cravings, food addiction includes the loss of control of eating behaviours and consistent excess food consumption, which is the definition of addiction. It can be defined as a physiological dependence, not just a physical ailment, as defined by the American Psychiatric Association (2000; Nelson et al., 1982).
Sugar addiction is a phenomenon that arises from a combination of factors including neurobiological, psychological and behavioural aspects. When sugar affects the brain’s reward system and alters pathways, it becomes intertwined with one’s emotions and habits, which can lead to behaviours resembling addiction (American Psychiatric Association, 2000; Diagnostic and statistical manual of mental disorders (DSM-5)). Understanding these mechanisms is crucial for addressing the rising concerns about sugar intake and its impact on public health.
The idea that sugar can act as a substance is similar to how the brain reacts to drugs. There are similarities between the areas of the brain that respond to rewards and those activated by substances (Hoebel, 1985; Hernandez & Hoebel, 1988; Kelley et al., 2002; Le Magnen, 1990; Volkow & Wise, 2005; Wise, 1989). The brain’s reward system, the dopamine pathway, plays a crucial role in reinforcing behaviours essential for survival, such as eating. However, the modern abundance of sugary foods might exploit this evolutionary system (Kalivas and Volkow, 2005; Kelley et al., 2005; Koob and Le Moal, 2005; Mogenson and Yang). The World Health Organisation (WHO) states that habits formed due to reputed behaviour are often a response to one’s environment. If a person regularly consumes sugary foods, the brain becomes used to the routine, thus making it difficult to break the consumption routine.
THERAPIES OF ADDICTION
Current Therapies
Drug therapy is an important component in treating individuals suffering from addictions. This approach involves the use of medications that act upon various brain pathways and neurotransmitter systems that can help in reducing withdrawal symptoms, cravings, and the reinforcing effects of substances. Moreover, different medications are used for different drug addictions (Badawy, 1999).
For alcohol users, Disulfiram is commonly used as this medication causes aversive reaction when combined with alcohol such as nausea and vomiting. In a 1992 study, researchers found that patients who took Disulfiram in a supervised setting drank significantly less than those who did not (Chick et al., 1992). However, a major downside of the Disulfiram treatment is the low compliance with the Disulfiram regimen, which is why researchers recommend an appropriate form of supervision in order to ensure that the ingestion of the Disulfiram is consistent (Brewer, 1987). There are concerns of the prescription that has a risk of adverse events and is potentially lethal, but it is a matter of weighing the efficacy of Disulfiram and the seriousness of the illness versus the toxicity of the drug, it is also important to note that Disulfiram has a moderate record of adverse effects (Chick, 1999).
Another drug treatment for alcohol consumers is Naltrexone. This treatment can be used to treat alcohol and opioid addiction; it works by blocking the brain’s opioid receptors which in return reduces the pleasurable and reinforcing effects of alcohol. A systematic review analysed multiple studies and came to the conclusion that Naltrexone was effective in increasing abstinence rates and reducing alcohol consumption (Kean Loon Ng et al., 2014). Naltrexone may be a more effective treatment due to its higher abstinence rates in comparison to Disulfiram because Naltrexone does not have the same negative aversive reactions.
An alternative drug used for opioid addiction is Methadone which is a long-acting opioid agonist that helps reduce withdrawal symptoms and cravings. It’s often used as a substitute for illicit opioids and is administered under medical supervision. It functions by interacting with the brain’s mu-opioid receptors. As a full agonist, it activates these receptors, alleviating withdrawal symptoms and cravings without producing intense euphoria. The half-life of Methadone is 8-59 hours. Therefore, due to its long half-life, it allows it to be used in the treatment of opioid dependence as it can be made into a once-daily dosage formulation. On the contrary, a drawback of this long half-life is prolonged intervals of toxicity which may last several days after contact with the medication requiring extended care (Anderson & Kearney, 2000). A study examined the effectiveness of Methadone Maintenance Treatment by assessing program factors, and patient characteristics, and found that Methadone reduced opioid use and improved social functioning (Simpson et al., 1997). However, one of the major issues with this treatment is the number of overdose deaths. A review found that the cause of these deaths was due to the Methadone being contaminated with Buprenorphine (Taxman et al., 2016). After reviewing the available evidence researchers found that measures can be taken to promote safer use of Methadone such as the need to educate and guide patients on Methadone safety, use of electrocardiography to identify people at greater risk for Methadone-associated arrhythmia, use of alternative opioids in patients at high risk of complications related to corrected electrocardiographic QTc interval prolongation, careful dose initiation and titration of Methadone, and diligent monitoring and follow-up (Chou et al., 2014).
To help combat nicotine addiction, Nicotine Replacement Therapy (NRT) is commonly used. This therapy includes products like nicotine gum, patches, inhalers etc. to help manage nicotine cravings while gradually reducing nicotine intake. A study found that only about 18% of smokers quitted smoking after one year, meaning that NRT alone might not lead to successful long-term cessation for all individuals (Fiore et al., 2003). NRT can have multiple physical side effects too. A further drug therapy used to treat smoking addiction is Varenicline, it works by activating nicotinic acetylcholine receptors when nicotine reaches them, and this leads to pleasure and addiction, a partial nicotine receptor agonist (Varenicline) which reduces withdrawal symptoms, cravings while it also reduces the rewarding effects of nicotine. The effectiveness of Varenicline therapy was shown in a study comparing this therapy with NRT for smoking cessation and they were found to be more likely to quit smoking, compared with patients prescribed NRT. This difference persisted over time, lasting as long as 4 years (Kotz D et al., 2014). It is important to be aware that all drug therapies have side effects that can cause physical harm. Therefore the choice of medications should be based on individual needs, medical history, and the type of addiction.
In addition to pharmacological treatment options, there are numerous behavioural therapy and psychotherapy options available. Psychotherapy can address both substance and non-substance addictions. Cognitive-Behavioral Therapy (CBT), the most used psychotherapeutic approach, centres on recognizing and modifying the thoughts, emotions, and behaviours that contribute to addictive patterns (Hong, 2017). The community reinforcement approach (CRA), which specifically targets alcoholism, aims to shift the rewards from drinking to those from maintaining sobriety (W. R. Miller, 1999). Another valuable behavioural therapy is aversion therapy. By altering the rewards associated with addiction and linking them to unpleasant experiences, the brain starts to associate the harmful behaviour with negative feelings.
Future Directions
Due to the high relapse rates, research continues to be conducted to find more effective treatment options. The use of classic “psychedelics” is one of the most promising reintroduced treatments for SUD. Classic psychedelics are a group of psychoactive drugs including lysergic acid diethylamide (LSD), psilocybin, N-dimethyltryptamine (DMT), and mescaline. These compounds can alter perception, cognition, and emotion (Lauren, 2022).
Psilocybin, a compound found in “psychedelic” mushrooms, has been shown, for example, to reduce heavy drinking by 83% when combined with psychotherapy (Bogenschutz MP, 2022). Moreover, the same study demonstrated that eight months after the first dose, 48% of those who received psilocybin stopped drinking altogether (Bogenschutz MP, 2022).
The classic “psychedelic” LSD has shown similar results. Since LSD was first synthesised in 1938, research has demonstrated its effectiveness in treating addiction in psychotherapeutic settings. One meta-study looked at six clinical trials between 1966 and 1970, finding that of those who had taken LSD to treat their alcoholism, 59% decreased their alcohol consumption, compared to 38% who did not take the drug (Krebs, 2012). Furthermore, participants who took LSD, in addition to therapy, were 15% more likely to remain sober six months after leaving treatment (Chant, 2012).
Non-invasive brain stimulation, which is the use of intense pulses of electric current delivered to the head, is an alternative field that is also currently being explored to treat addiction. The induced electric field triggers an action potential in the brain and alters neural activity (Frontiers, 2019). Many studies have addressed whether addiction could be alleviated by non-invasive brain stimulation (NIBS) techniques with contradicting findings. Nevertheless, a meta-analysis found compelling evidence for the viability of using NIBS to remit substance-addictive behaviour (Tianye Ma, 2019).
DISCUSSION
This paper discussed the multiple theories, types and treatments of addictions. The two main theories describing the prevalence of addiction mentioned in this paper are: the addiction cycle and the Incentive-Sensitization Theory. Although some resources reveal that the addiction cycle only applies to drug and alcohol addiction, it may indeed also be reflected on behavioural addictions with the same mechanism; the reason is that people may not only consume addictive substances but also engage in addictive behaviours. Similar to the action of intaking an addictive substance, when people are using certain social media applications, a sense of pleasure may occur, causing them to repeat certain behaviours again and again.
There are various substance and behavioural addictions, the main disorders explored were alcoholism, heroin and cocaine addiction, social media, and sugar. However, gambling disorder is the only listed behavioural addiction in the DSM-V. The Diagnostic and Statistical Manual has been criticised for its reductionist approach to diagnosing mental disorders, and does not recognise social media and sugar as addictions. Social media has only emerged within the past two decades. This conveys how important addiction research is, to collect data about potential disorders so that they may be recognised and treated.
Due to the widespread presence of addiction in society many treatments have been developed. The most common being drug and behavioural therapies. For example Disulfiram and Naltrexone are used to tackle the withdrawal symptoms and cravings of alcohol respectively. Nicotine Replacement Therapy (NRT) is commonly used to treat nicotine addiction through the replacement of nicotine found in cigarette form to nicotine gum, patches, inhalers etc. Typically, addictions are not only treated pharmacologically but rather in addition to other behavioural therapies. Three of the most common therapies used are CBT, CRA and aversion therapy. Despite the variety of treatments available, the relapse rate remains high which has led to research into alternative methods for the treatment of addiction. Early research into “psychedelics” such as Psilocybin and LSD have been shown to be very promising in treating addiction. Some NIBS techniques have also been shown to help.
Addiction permeates throughout many societies affecting millions, making research crucial to improving and healing communities, economies and individual lives. Especially in low-income families and communities, access to treatment can be difficult due to how expensive it can be. Untreated mental health issues lead to deteriorating overall health, which impacts the economy as it correlates with more deaths, a less apt workforce, and less efficiency across industries, therefore impacting economies on a macro scale, such as in areas of Latin America and North America.
This paper provides only a brief introduction into what addiction is as well as the past and current research being conducted and therefore has multiple limitations. This paper is an analytical one, mentioning conclusions found from secondary studies with no primary research having been conducted in its completion. Furthermore, there are multiple external limitations in the research of addiction that affect the conclusions of the paper. The conclusions from the newer research mentioned such as the use of “psychedelics” and NIBS are limited as they are still very regulated without a substantial amount of studies having been conducted. More research in these areas is being conducted, since data is needed across various demographics in these areas to make results more generalizable.
One of the main issues with addiction is how those who suffer from it can be unable or unwilling to seek help, due to socioeconomic barriers or due to the stigmatisation of mental health issues such as addictions. As aforementioned, addicts specifically in low income families or communities, may find it more difficult to access therapies due to a larger deficit in resources. It is essential that the current therapies on the market be made accessible to all who are susceptible to addiction whilst new research continues into more effective treatment options.
CONCLUSION
In conclusion, the study of addiction is a complex and multifaceted field that has significantly evolved over the years. The addiction cycle provides a thorough framework for comprehending how addiction develops and continues through time. The stages of the cycle, binge/intoxication phase, withdrawal/negative affect phase and the preoccupation/anticipation stage, emphasise the progression of addiction. The Incentive-Sensitization Theory postulates that repeated exposure to a rewarding stimulus, such as drugs, can lead to changes in the brain’s reward circuitry. This results in an enhanced sensitivity to cues associated with the reward, even as the actual pleasure or “liking” response to the reward may diminish over time.
Addiction types demonstrate how complex human nature and behaviour are. We can see how vulnerable individuals can be. Alcohol is a widely prevalent addiction and can take over one’s life. It can lead to irreversible brain damage. Social media has become a widely spread behavioural addiction in the last few years. It can captivate one’s emotions and control minds, creating mental health problems, especially among adolescents. Sugar “craving” has many features that can be considered as a type of addiction, however it has not been, yet, formally included to any stage of clinical addiction. However sugar craving can evolve from a certain form into a psychological addiction resembling substance dependence. These emphasise the importance of prevention and treatment of various forms of addiction. With modern technology, new strategies can be developed to address both the physiological and physical aspects of these problems and promote healthier lifestyles.
Overall, addictions are currently treated through medications, behavioural therapy and psychotherapy, often synergistically. Researchers are also exploring novel treatments involving “psychedelics” and NIBS, one of the reasons being due to the current high relapse rates. Addiction affects societies globally, necessitating vital research. Treatment access challenges, especially in low-income areas, exacerbate mental health issues, leading to declining well-being that hampers communities.
Altogether, this paper briefly introduces addiction and current research but has limitations. It’s an analytical piece citing secondary studies; no primary research is conducted. External constraints in addiction research affect conclusions. Newer research, like “psychedelics” and NIBS, has limited conclusions due to regulation and insufficient studies. Ongoing research aims to gather diverse demographic data for broader results. A significant challenge is that stigma and socioeconomic barriers can prevent seeking help for addiction and mental health issues.
References
Alcohol Change UK (2020). Alcohol Statistics. [online] Alcohol Change UK. Available at: https://alcoholchange.org.uk/alcohol-facts/fact-sheets/alcohol-statistics.
Alcohol Change UK. (n.d.). Is alcohol addictive? [online] Available at: https://alcoholchange.org.uk/alcohol-facts/fact-sheets/is-alcohol-addictive.
American Addiction Centers (2019). What is process addiction & types of addictive behaviours? [online] American Addiction Centers. Available at: https://americanaddictioncenters.org/behavioral-addictions.
An, H., He, R.-H., Zheng, Y.-R. and Tao, R. (2017). Cognitive-Behavioral Therapy. Advances in Experimental Medicine and Biology, 1010, pp.321–329. doi:https://doi.org/10.1007/978-981-10-5562-1_16.
Anderson, I.B. and Thomas E Kearney, T. (2000). Use of methadone. Western Journal of Medicine, [online] 172(1), pp.43–46. doi:https://doi.org/10.1136/ewjm.172.1.43.
Anon, (2023). Exploring Addiction: Why Is Alcohol Addictive? [online] Available at: https://www.addictiongroup.org/alcohol/addictive/ [Accessed 18 Aug. 2023].
Avena, N.M., Long, K.A. and Hoebel, B.G. (2005). Sugar-dependent rats show enhanced responding for sugar after abstinence: Evidence of a sugar deprivation effect. Physiology & Behavior, [online] 84(3), pp.359–362. doi:https://doi.org/10.1016/j.physbeh.2004.12.016.
Avena, N.M., Rada, P. and Hoebel, B.G. (2008). Evidence for sugar addiction: Behavioral and neurochemical effects of intermittent, excessive sugar intake. Neuroscience & Biobehavioral Reviews, 32(1), pp.20–39. doi:https://doi.org/10.1016/j.neubiorev.2007.04.019.
Aversion therapy. Council on Scientific Affairs. (1987). JAMA, [online] 258(18), pp.2562–2566. Available at: https://pubmed.ncbi.nlm.nih.gov/3312661/ [Accessed 18 Aug. 2023].
Badawy, A.A.-B. . (1999). Tryptophan metabolism in alcoholism. Nutrition Research Reviews, doi:https://doi.org/10.1079/nrr200133 https://pubmed.ncbi.nlm.nih.gov/19087401/.
Baik, J.-H. (2013). Dopamine Signaling in reward-related behaviors. Frontiers in Neural Circuits, 7(152). doi:https://doi.org/10.3389/fncir.2013.00152.
Banyan Treatment Center. (2021). Difference Between Cocaine And Heroin. [online] Available at: https://www.banyantreatmentcenter.com/2021/07/27/cocaine-and-heroin-differences-texas/.
Berridge, K.C. and Kringelbach, M.L. (2015). Pleasure Systems in the Brain.
Berridge, K.C. and Robinson, T.E. (2016). Liking, wanting, and the incentive-sensitization theory of addiction. American Psychologist, [online] 71(8), pp.670–679. doi:https://doi.org/10.1037/amp0000059.
Bogenschutz, M.P., Ross, S., Bhatt, S., Baron, T., Forcehimes, A.A., Laska, E., Mennenga, S.E., O’Donnell, K., Owens, L.T., Podrebarac, S., Rotrosen, J., Tonigan, J.S. and Worth, L. (2022). Percentage of heavy drinking days following psilocybin-assisted psychotherapy vs placebo in the treatment of adult patients with alcohol use disorder. JAMA Psychiatry, 79(10). doi:https://doi.org/10.1001/jamapsychiatry.2022.2096.
Boston, 677 H.A. and Ma 02115 +1495‑1000 (2021). Cravings. [online] The Nutrition Source. Available at: https://www.hsph.harvard.edu/nutritionsource/cravings/.
Chant, I. (2012). Curing Addicts with Acid. Scientific American Mind, [online] 23(3), pp.12–12. doi:https://doi.org/10.1038/scientificamericanmind0712-12b.
Chapter 2 Preview. (n.d.). Available at: https://addiction.surgeongeneral.gov/sites/default/files/chapter-2-neurobiology.pdf.
Chou, R., Cruciani, R.A., Fiellin, D.A., Compton, P., Farrar, J.T., Haigney, M.C., Inturrisi, C., Knight, J.R., Otis-Green, S., Marcus, S.M., Mehta, D., Meyer, M.C., Portenoy, R., Savage, S., Strain, E., Walsh, S. and Zeltzer, L. (2014). Methadone Safety: A Clinical Practice Guideline From the American Pain Society and College on Problems of Drug Dependence, in Collaboration With the Heart Rhythm Society. The Journal of Pain, 15(4), pp.321–337. doi:https://doi.org/10.1016/j.jpain.2014.01.494.
Clay, S.W., Allen, J. and Parran, T. (2008a). A review of addiction. Postgraduate Medicine, [online] 120(2), pp.E01-07. doi:https://doi.org/10.3810/pgm.2008.07.1802.
Clay, S.W., Allen, J. and Parran, T. (2008b). A review of addiction. Postgraduate Medicine, [online] 120(2), pp.E01-07. doi:https://doi.org/10.3810/pgm.2008.07.1802.
Cleveland Clinic. (2022). Basal ganglia: What it is, function & anatomy. [online] Available at: https://my.clevelandclinic.org/health/body/23962-basal-ganglia.
Crone, E.A. and Konijn, E.A. (2018). Media Use and Brain Development during Adolescence. Nature Communications, [online] 9(1). doi:https://doi.org/10.1038/s41467-018-03126-x.
Hasin, D.S., O’Brien, C.P., Auriacombe, M., Borges, G., Bucholz, K., Budney, A., Compton, W.M., Crowley, T., Ling, W., Petry, N.M., Schuckit, M. and Grant, B.F. (2013). DSM-5 Criteria for Substance Use Disorders: Recommendations and Rationale. American Journal of Psychiatry, [online] 170(8), pp.834–851. doi:https://doi.org/10.1176/appi.ajp.2013.12060782.
Healthline. (2012). Wernicke-Korsakoff Syndrome: Risks, Causes, Symptoms, and More. [online] Available at: https://www.healthline.com/health/wernicke-korsakoff-syndrome#causes.
Hou, Y., Xiong, D., Jiang, T., Song, L. and Wang, Q. (2019). Social Media addiction: Its impact, mediation, and Intervention. Cyberpsychology: Journal of Psychosocial Research on Cyberspace, [online] 13(1), pp.1–17. doi:https://doi.org/10.5817/cp2019-1-4.
https://www.genesisrecovery.com/. (n.d.). The Stages of Addiction. [online] Available at: https://www.genesisrecovery.com/the-stages-of-addiction/ [Accessed 26 Aug. 2023].
Jacobson, R. (2016). A One-Dose Psychedelic Fix for Addiction? Scientific American Mind, 28(1), pp.10–11. doi:https://doi.org/10.1038/scientificamericanmind0117-10.
Johansen, L., Liknaitzky, P., Nedeljkovic, M., Mastin-Purcell, L. and Murray, G. (2022). The psychological processes of classic psychedelics in the treatment of depression: a systematic review protocol. Systematic Reviews, 11(1). doi:https://doi.org/10.1186/s13643-022-01930-7.
Jones, G., Ricard, J.A., Lipson, J. and Nock, M.K. (2022). Associations between classic psychedelics and opioid use disorder in a nationally-representative U.S. adult sample. Scientific Reports, 12(1). doi:https://doi.org/10.1038/s41598-022-08085-4.
Lenoir, M., Serre, F., Cantin, L. and Ahmed, S.H. (2007). Intense Sweetness Surpasses Cocaine Reward. PLoS ONE, [online] 2(8), p.e698. doi:https://doi.org/10.1371/journal.pone.0000698.
Liu, J. and Li, J. (2018). Drug addiction: a curable mental disorder? Acta Pharmacologica Sinica, [online] 39(12), pp.1823–1829. doi:https://doi.org/10.1038/s41401-018-0180-x.
Lyden, J. and Binswanger, I.A. (2019). The United States opioid epidemic. Seminars in Perinatology, [online] 43(3), pp.123–131. doi:https://doi.org/10.1053/j.semperi.2019.01.001.
Ma, T., Sun, Y. and Ku, Y. (2019). Effects of Non-invasive Brain Stimulation on Stimulant Craving in Users of Cocaine, Amphetamine, or Methamphetamine: A Systematic Review and Meta-Analysis. Frontiers in Neuroscience, 13. doi:https://doi.org/10.3389/fnins.2019.01095.
Miller, W.R., Meyers, R.J. and Hiller-Sturmhöfel, S. (1999). The community-reinforcement approach. Alcohol Research & Health: The Journal of the National Institute on Alcohol Abuse and Alcoholism, [online] 23(2), pp.116–121. Available at: https://pubmed.ncbi.nlm.nih.gov/10890805/ [Accessed 18 Aug. 2023].
National Institute on Alcohol Abuse and Alcoholism (2021). The Cycle of Alcohol Addiction | National Institute on Alcohol Abuse and Alcoholism (NIAAA). [online] www.niaaa.nih.gov. Available at: https://www.niaaa.nih.gov/publications/cycle-alcohol-addiction.
National Institute on Drug Abuse (2020a). Drugs and the Brain. [online] National Institute on Drug Abuse. Available at: https://nida.nih.gov/publications/drugs-brains-behavior-science-addiction/drugs-brain.
National Institute on Drug Abuse (2020b). Treatment and Recovery. [online] National Institute on Drug Abuse. Available at: https://nida.nih.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery.
NHS (2021). Addiction: what is it? [online] nhs.uk. Available at: https://www.nhs.uk/live-well/addiction-support/addiction-what-is-it/.
NIAAA (2022). The Cycle of Alcohol Addiction | National Institute on Alcohol Abuse and Alcoholism (NIAAA). [online] www.niaaa.nih.gov. Available at: https://www.google.com/url?q=https://www.niaaa.nih.gov/publications/cycle-alcohol-addiction&sa=D&source=docs&ust=1693063920378434&usg=AOvVaw3Fg_NhNBtNB9j9yNvFI6-h [Accessed 26 Aug. 2023].
Office of the Surgeon General, A.S. for H. (ASH) (2019). Addiction and Substance Misuse Reports and Publications. [online] HHS.gov. Available at: https://www.hhs.gov/surgeongeneral/reports-and-publications/addiction-and-substance-misuse/index.html.
Poland, J. and Graham, G. (2011). Addiction and Responsibility. [online] Google Books. MIT Press. Available at: https://books.google.ro/books?hl=ro&lr=&id=mc7xCwAAQBAJ&oi=fnd&pg=PA21&dq=Drug+Addiction+as+Incentive+Sensitization&ots=f8keNq7GhU&sig=vBVirWmeWJTNBoLWQZgWhpGg2EE&redir_esc=y#v=onepage&q=Drug%20Addiction%20as%20Incentive%20Sensitization&f=false [Accessed 16 Aug. 2023].
Promises Behavioral Health. (2017). Why Is Alcohol Addictive? The Science Behind Alcoholism. [online] Available at: https://www.promises.com/addiction-blog/why-is-alcohol-addictive-the-science-behind-alcoholism/.
Ritchie, H. and Roser, M. (2018). Alcohol consumption. [online] Our World in Data. Available at: https://ourworldindata.org/alcohol-consumption.
Robinson, L. and Smith, M. (2023). Social media and mental health. [online] HelpGuide.org. Available at: https://www.helpguide.org/articles/mental-health/social-media-and-mental-health.htm.
Robinson, M.J.F., Fischer, A.M., Ahuja, A., Lesser, E.N. and Maniates, H. (2015). Roles of ‘Wanting’ and ‘Liking’ in Motivating Behavior: Gambling, Food, and Drug Addictions. Behavioral Neuroscience of Motivation, 27, pp.105–136. doi:https://doi.org/10.1007/7854_2015_387.
Shenoy, S.S. and Lui, F. (2020). Biochemistry, Endogenous Opioids. [online] PubMed. Available at: https://www.ncbi.nlm.nih.gov/books/NBK532899/.
THE OPIOID CRISIS AND THE HISPANIC/LATINO POPULATION: AN URGENT ISSUE. (2020). Available at: https://store.samhsa.gov/sites/default/files/pep20-05-02-002.pdf.
US Department of Health and Human Services (2016). THE NEUROBIOLOGY OF SUBSTANCE USE, MISUSE, AND ADDICTION. [online] Nih.gov. Available at: https://www.ncbi.nlm.nih.gov/books/NBK424849/.
Volkow, N.D. and Boyle, M. (2018). Neuroscience of Addiction: Relevance to Prevention and Treatment. American Journal of Psychiatry, 175(8), pp.729–740. doi:https://doi.org/10.1176/appi.ajp.2018.17101174.
Warlow, S.M., Baumgartner, H.M., Freeland, C.M., Naffziger, E.E., Olney, J.J., Berridge, K.C. and Robinson, M.J.F. (2020). Sensitization of Incentive Salience and the Transition to Addiction. [online] Cambridge University Press. Available at: https://www.cambridge.org/core/books/abs/cambridge-handbook-of-substance-and-behavioral-addictions/sensitization-of-incentive-salience-and-the-transition-to-addiction/E904DBA2BA0DE15831A17D6A11F928F7.
Wiss, D.A., Avena, N. and Rada, P. (2018). Sugar Addiction: From Evolution to Revolution. Frontiers in Psychiatry, 9(30464748). doi:https://doi.org/10.3389/fpsyt.2018.00545.
World Health Organization (2020). Healthy Diet. [online] World Health Organisation. Available at: https://www.who.int/news-room/fact-sheets/detail/healthy-diet.