Supervised by: Jasmine Lee, BA (Hons) (Cantab.). Jasmine recently graduated from the University of Cambridge having studied Psychological and Behavioural Sciences. She did outreach work for Pembroke College as a student ambassador, and organised TEDx events as the co-president of TEDxCambridgeUniversity. She is currently studying for her masters in Developmental and Educational Psychology at University College London (UCL).
Abstract
This study reviewed available research on the description, variables, literature, and the risk factors that can lead to developing Dissociative Amnesia in the aftermath of trauma. These ranged from war and abuse to other biological or environmental factors. The study will also be covering the 6 forms of Dissociative Amnesia: selective, continuous, systematized, generalized, localized and fugue. The effect of psychological trauma on the brain leading to Dissociative Amnesia was also analyzed, as well as the impact of developing this trauma response on a patient’s daily life. Treatments explored in this study include psychopharmacological and somatic treatments, psychotherapeutic interventions, and neuropsychological rehabilitation.
Introduction
Dissociative Amnesia is a kind of condition which causes “inability to recall important personal information, usually of a traumatic or stressful nature, that is too extensive to be explained by ordinary forgetfulness” (Sharon, 2005). Formerly called “psychogenic amnesia”, Dissociative Amnesia is a disorder dissimilar to normal amnesia, as the memories are still present in the individual, however, they dwell deep within the brain of the person and cannot be recalled. These memories may resurface in the person if recalled due to remembrance or other factors ranging from seeing matter to the person’s environment.
Dissociative Amnesia occurs when there is overwhelming stress, trauma, or other factors that impact the brain. Dissociative Amnesia is a response to this problem. Due to the lack of profound understanding in the cause and aftermath of Dissociative Amnesia, this paper highlights the known and suggestions in order to combat Dissociative Amnesia. The proposed suggestions will directly benefit patients who are diagnosed with Dissociative Amnesia. Proposed ways to rehabilitate patients may be incorporated and used by neurotherapists and specialists to help heal and recuperate them.
There are different forms of memory loss identified, the 5 major forms of amnesia being localized, selective, continuous, systematized and generalized. Localized amnesia causes patients to become unable to remember a specific event or period of time. Generalized amnesia refers to the case in which a patient loses complete memory of their own identity and past experiences. Continuous amnesia occurs when a patient loses memory of events as they occur. Systematic amnesia includes the inability to recall information in a specific category. Finally, selective amnesia diagnoses patients with the inability to recall parts of a traumatic event or series of traumatic events, but are capable of remembering specific details.
In Dissociative Amnesia, the information lost would normally be part of conscious awareness and would be described as autobiographical memory (Spiegel, 2021). Dissociative Amnesia is caused by a number of events, most notably trauma. This could be trauma from a childhood memory or an adult one, however, these occurrences are typically brought on by war, injury, rape, natural disasters, and a number of social issues. Stress and depression caused by financial issues, marriage, death of a loved one or any other stress inducing problem in society may also lead to Dissociative Amnesia. Finally, epilepsy and other internal brain damage or diseases may lead to Dissociative Amnesia.
Background Information
Dissociative Amnesia is a typically trauma-induced condition that affects approximately 1% of men and 2.6% of women. It is categorized by the person being unable to remember or recall information, including places and people in their life. This includes the inability to recall certain aspects that a person may correlate to a traumatic event they have experienced, or forgetting arbitrary information about previous life history and/or personal details. Dissociative Amnesia is classified under the category of Dissociative Disorders; which are defined as disorders that impair or alter one’s state of cognitive operations, impacting consciousness, perception of identity or memory. The condition falls under six different labels depending on how it manifests in an individual.
Localized Dissociative Amnesia is determined when a specific traumatic event causes a person to forget any specific fragment of knowledge that a person attributes to the event (which may vary from case to case). An example of this is if a person who has experienced childhood trauma forgets the house they grew up in, the names of prominent people in childhood and activities that they partook in.
Selective Dissociative Amnesia is when there is a gap in the memory for a certain period of time, for instance when a person may recall some details from a series of traumatic events, but may forget a large portion. Selective and Localized amnesia may occur simultaneously.
Systematized Dissociative Amnesia is memory loss that relates to a specific area or entity, such as someone forgetting all memories that involve a specific person.
Continuous Dissociative Amnesia occurs in a series of forgotten events as they transpire, which may be triggered by a specific, initial event that kickstarts the continuous forgetting.
Generalized Dissociative Amnesia is when a person completely forgets every past experience and their own identity which may cause them to change their identity entirely, forgetting previously honed skills.
Dissociative Fugue is one of the rarest forms of this disorder, when a person sporadically forgets their identity and their surroundings; a person may be in one place at a point in time and find themselves at a different, unknown location at another time. Fugue is categorized more distinctly in DSM-V clauses as it is postulated to have a more prominent impact on an individual, depicted in scans showing less dorsolateral prefrontal cortex arousal than another form. This will be further explained in a later section.
Most recently in 2013, the DSM-V defined Dissociative Amnesia as “An inability to recall important autobiographic information, usually of a traumatic or stressful nature, that is inconsistent with ordinary forgetting.” The DSM-V distinguishes a difference between Dissociative Amnesia and typical amnesia, which eliminates information from the mind altogether as a result of disease or physical injury to the brain. In Dissociative Amnesia however, the memories are deeply buried in the subconscious, but still subsist.
The DSM-V also notes,”Dissociative Amnesia most often consists of localized or selective amnesia for a specific event or events; or generalized amnesia for identity and life history” [1], [3]:298, Code 300.12. The former Code 300.12 and 300.13 clauses within the DSM-V categorized Dissociative Amnesia forms into either Localized Amnesia, Selective Amnesia and Dissociative Fugue. Contrarily, in the most current version, Continuous and Systematized Dissociative Amnesia are recognised as facets of the disorder. Previously, Dissociative Fugue was implied to be one of the common branches of the disorder, but is now more segregated as a more rigorous form of the disorder, which is due to the evidently greater impact it has on the lives of individuals who experience it because of the symptomatic effects.
A study shown in Figure A shows two individuals – one with Dissociative Fugue (b) and another with an undefined form (a) of Dissociative Amnesia – who undertook a series of recognition tests with people from their past. In simplified terms, the red indicates where the brain is working to recall the memories that are still apparent, shown in the prefrontal cortex (Figure C). The yellow indicates the hippocampus (Figure C) where the memory is still apparent.
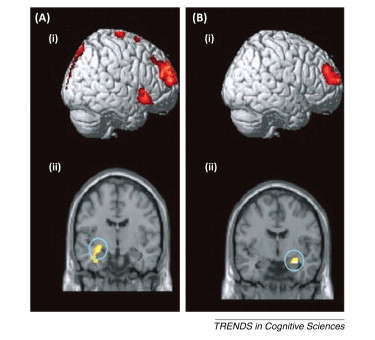
Figure A
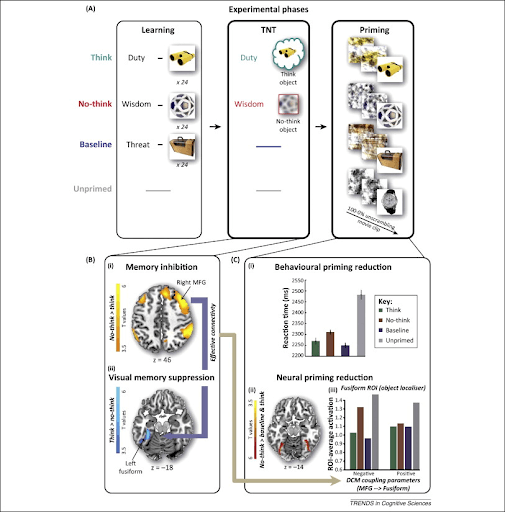
Figure B
Figure B further demonstrates the brain activity within the hippocampus and the prefrontal cortex. It is shown that there is much less prevalent brain activity in Patient B, in terms of prefrontal cortex arousal, reaction time and suppression of memory. Thus, the study suggests that the patient with Dissociative Fugue shows stronger impact on the suppression of memory (comparatively), but less on the stimulation of the prefrontal cortex, demonstrating how Dissociative Fugue impacts the brain and therefore the individual, more prominently.
Flaws in the study:
Definitions https://my.clevelandclinic.org/health/diseases/9789-dissociative-amnesia
https://www.medicalnewstoday.com/articles/dissociative-amnesia#types
Risk Factors
Oftentimes, when exposed to adverse experiences, such as abuse, children are more likely to develop Dissociative Amnesia and block out the trauma (Joseph, 1999). This occurs for a number of reasons. Firstly, children’s hippocampi are not completely formed, as the hippocampus does not complete myelination until adulthood (Joseph, 1999). Myelination in the production of myelin that cover the axons and allow for a smoother transition of action potentials. Therefore it is more prone to undergoing neuroplastic alterations. Additionally, the immaturity of the corpus callosum before the age of five prevents information and memories from transferring between the right and left hemispheres (Joseph, 1999). However, the brain not being fully formed is not the only reason why children are more susceptible to Dissociative Amnesia. Unfortunately, trauma is sometimes caused by a child’s caregiver. The Betrayal Trauma Theory, formulated by psychology professor J.J. Freyd, states that the brain adapts to threatening situations caused by a loved one, through Dissociative Amnesia (Wolf & Nochajski, 2013).
A case study conducted by Sroufe and Duggal suggests the validity of the Betrayal Trauma Theory. They performed a longitudinal study to observe the effects of early childhood trauma on the development of Dissociative Amnesia. The subject was referred to as the pseudonym “Laura.” Laura’s parents shared joint custody after their divorce, however, Laura’s teacher began noticing strange sexualized behavior. During an interview with the researchers, Laura’s mother (known under the pseudonym “Ms. Miller”) revealed that “Laura would cry, tantrum, and have nightmares when she went to stay with her father” (Sroufe & Duggal, 1998). It is reported that the subject’s father would go into her bed and touch her while she begged him to stop. Laura was around four at the time. Soon afterward, Laura began therapy and displayed awareness of what had happened to her. For years later, she told teachers and friends that she had been sexually abused, however, third grade marks the last childhood record of memory of her trauma.
At the age of sixteen Laura was assessed with a health survey. She indicated on the survey that she had never been sexually abused. Although this discrepancy could have been caused by an unwillingness to converse, the interviewer expressed that Laura was “talkative and open about her life and was not uncomfortable answering any of the questions” (Sroufe & Duggal, 1998). The Kiddie Schedule for Affective Disorders and Schizophrenia taken a year later showed similar results. When asked whether she had ever gone through any terrible and unusual experiences, Laura replied that she had not. Because Laura was so young when she was abused and because her abuser was someone she lived with from time to time, her brain had to essentially forget about the abuse that had happened to her. According to Freyd, for Laura to “withdraw from a caregiver [she is] dependent on would further threaten [her] life, both physically and mentally” (Freyd, 2003).
Age is not the only contributing factor to the development of Dissociative Amnesia. The environment plays a role as well. For example, repeated disclosure of the events that took place have a positive effect on memory (Wolf & Nochajski, 2013). Because childhood abuse is an offense punishable by law, children who experience it often have to go through the legal system. A study by Alexander et al. shows that “legal involvement might be associated with elaborative rehearsal, which facilitates long-term retention” (Alexander et al., 2005). Unfortunately, not all children get the opportunity to share their story. Due to cultural standards, males are often less likely to be vulnerable with others. In the same study, Alexander et al. found that the less they talk about their abuse, the more likely they are to forget it. However, other researchers have found a contrasting gender effect. A 1997 study found that 25.4% females experienced amnesia versus 7.1% of males (Melchert & Parker, 1997). These varying results conclude that there is not enough evidence to prove that one gender is more susceptible than the other, but that the ability to disclose can help with memory.
Stressful or traumatic events in general for any age can be a risk factor. Examples include natural disasters (e.g. hurricanes, tornadoes), exposure to war, a vehicle incident, or the passing of someone who had been close to the individual. In a study which looked at a man who had endured the 2011 Tōhoku earthquake and tsunami, the patient visited the clinic of the Department of Psychiatry, Saitama Medical University Hospital on November 1st, 2016 (Odagaki, 2017). The Abbreviated Mental Test (AMT) as well as general physical and neurological examinations were performed on him. The only questions he could not answer were the ones pertaining to his age and date of birth. His memory was found to be completely lost until March 11th, 2011, the date of the 2011 Tōhoku earthquake and tsunami. Short term memory was prominent for he could remember events that he had encountered subsequent to the natural disaster. Prior to the disaster, the patient had lost all autobiographical memory and later on wanted to shed light onto his personal identity. This case essentially suggests that Dissociative Amnesia, as well as other dissociative spectrum disorders, need to be taken into account where victims of disaster are analyzed.
Furthermore, in a study by Dr. Nejad and Dr. Farahati (2007), which took place between January and September 2005, at Beheshti Psychiatric Hospital, Kerman, Iran, the severity of Post-Traumatic Stress Disorder (PTSD) was measured by the Davidson PTSD scale and dissociative symptoms were analyzed using the dissociative experience scale (DES). The dissociative disorder interview schedule (DDIS) was used to analyze Dissociative Disorders. The most ubiquitous Dissociative Disorder was Dissociative Amnesia. The conclusion of this case was veterans with chronic PTSD may have a follow up of Dissociative Disorders.
These being risk factors, it is also crucial to mention that having a risk factor does not imply that an individual would develop Dissociative Amnesia nor does not having a risk factor determine that the individual will not have the condition (DoveMed, 2020). There is a lack of evidence for determining protective factors.
Impacts
Neurobiological
The primary neurobiological factors that cause Dissociative Amnesia are heightened stimulation of the hippocampus, amygdala, and prefrontal cortex (Bidzan, 2017).
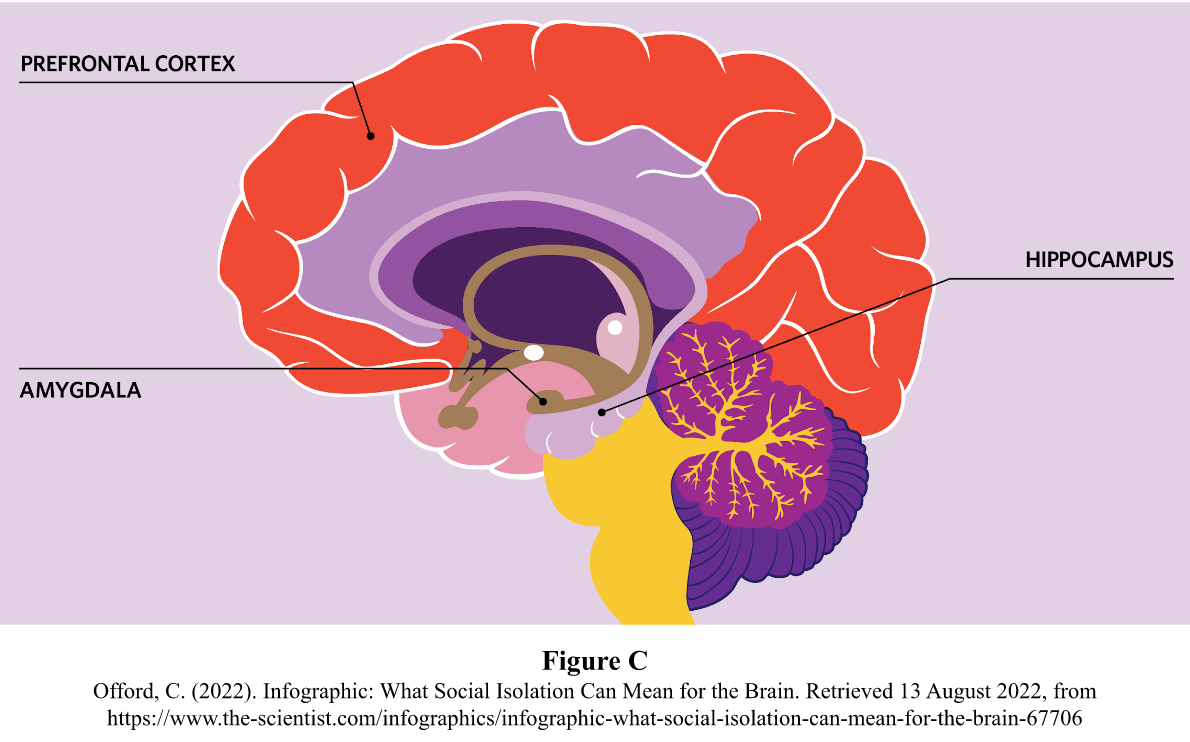
As the hippocampus is a structure that typically plays a significant role in the storage of long-term memory, memory deficiencies like Dissociative Amnesia can be brought on by stress-induced abnormalities with hippocampal activation and arousal. In a state of hyperarousal, correct hippocampus functions are deregulated, which may result in memory loss. The hypothalamic-pituitary-adrenal (HPA) axis regulates the release of “stress hormones”, particularly glucocorticoids (the principal form of which produced in humans is cortisol), which are secreted in response to distressing factors during physiologically induced states of stimulation.
Due to a negative feedback mechanism, excessive release is usually prevented and the response ends – this does not occur when glucocorticoid secretion is prolonged or especially intense (McEwen, 1993). Maladaptive responses to stressors like psychological trauma can result in excessive or extended cortisol release as well as a fear-based memory of the stressful stimuli that is easily reactivated by other stressors. Cortisol dysfunction is caused by prolonged cortisol secretion, as a result of an inadequate coping mechanism for acute stress (Hannibal & Bishop, 2014).
Excessive and long-term deregulation of the HPA axis can impair hippocampus function. Rapid and extended cortisol secretion can inhibit neuronal activity involved in memory and learning and cause degeneration of the hippocampus (Joseph, 1999). A decrease in hippocampus volume was seen in patients with Dissociative Amnesia who had experienced childhood trauma, particularly those who had experienced emotional neglect (Dimitrova et al., 2021). Interestingly, there was no significant negative correlation between hippocampal volumes and emotional, physical and sexual abuse subscales. However, this study had limitations: it only included Dissociative Identity Disorder (DID) patients who also experienced Dissociative Amnesia, and the sample was exclusively female.
The processing of memories and feelings associated with fear is mainly dictated by the amygdala. When a stimulus enters the brain, it is neutral and neither “important” nor “unimportant”- its meaning is determined by the emotion that is attached to it. Information is given an emotional component in the amygdalae before having an impact on memory. The amygdala likely controls whether a stimulus that enters an organism is registered and processed, whether it will acquire emotional meaning, and whether it will subsequently be remembered (Phelps & LeDoux, 2005).
In a study by Rauch et al. (2000), the masked-faces paradigm was utilized, in which subjects were presented brief expressions of fear or joy followed by more prolonged neutral expressions.
The neutral faces “masked” the happy or frightening faces from conscious awareness since they were not displayed for long enough for mindful observation to occur. The PTSD group displayed noticeably more amygdala activity than the control group in the masked-fearful face condition as compared to masked-happy face condition. In this way, PTSD-affected individuals were shown to have greater amygdala activation in response to general negative stimuli, and hippocampal function is impeded when the amygdala receives an excessively high level of stimulation (Akirav & Richter-Levin, 2006).
Studies on emotional recognition in PTSD-affected individuals have used a few types of experimental design; some making use of emotional recognition tasks where participants identify emotions on adult faces; others using attentional bias tasks where a dot appears on either side of a screen that shows both an emotive and a neutral face. When the dot is placed on the same side as the emotional face, participants respond more quickly due to attentional bias toward the emotional face. Considerable research has also looked into brain activity while processing emotions (Bérubé et al., 2021). Overall, the evidence concludes that people who have Dissociative Amnesia and other severe post-stress disorders have shown that they have worsened recognition of certain emotions, particularly fear and sadness. According to psychological research, these emotional states are perceived with a significantly reduced degree of accuracy and sensitivity (Poljac et al., 2011).
Studies using positron emission tomography (PET) scans which measure the metabolism of the brain using radioactive tracers, suggest that the prefrontal cortex, which controls cognition skills, is a factor in the mechanisms underlying Dissociative Amnesia. Brand et al. (2009) examined the consumption of glucose in various brain regions in affected individuals – it was discovered that the metabolic activity of the prefrontal lobes is inhibited by memory disorders brought on by stressful situations.
Daily Life
The basis of Dissociative Amnesia is that someone with it can also have it adjacent to a form of this amnesia known as Dissociative Fugue. This implies that a person will not have any recollection of their past or themselves as an individual. In a study conducted by Dr. Tobechukwu Clouden (2020), the case of a 20-year old woman was presented. The patient had PTSD and Schizoaffective Disorder suggesting that Dissociative Disorders can exist with psychotic disorders. When in the ER, she was asked to recollect what happened and a story was pieced together in which she had gotten kicked out of her group home since she aged out of it and had encountered being close to being raped and adopting a child from a man involved in substance abuse. This was a story that had formed in her mind due to immense stress. This fear of being kicked out led to paranoia and self-dialogging, believing that items of her property were stolen, going missing from the group home, and being found wandering alone on a highway. The connection between stressors and Dissociative Amnesia is clear here. What is unique about this case is the replacement of the amnesic events. The story with the man whose child she adopted could be related to past traumatic events in her life. The child could represent her and the man, her father. Her mother, who the patient mentioned, joined her and the child. Following this idea, the reason for her mother being in the story could represent her desire to have had moral support from her mother. Her mother had also been known to have been a major stressor and the patient could not recall what the ongoing conflict was. Another idea was that the patient saving the child was an altruistic response but it is also possible that the substitution of events was caused by amnesia due to the patient’s trauma and stress.
According to a study conducted by Dr. Igwe (2013), Dissociative Fugue, a subtype of Dissociative Amnesia (Cuncic, 2020), coexists with a major stressor in an individual’s life. In this particular case, a 28 year old man, who had been missing for 10 days, was found with no recollection of how he came to be in his found location. It was then found that the patient had seen a human skeleton across his desk 10 nights prior to his finding, and that the room had become unstable segueing into what was described as overwhelming fears. Stressors that had been prevalent were economic and academic. The patient’s mood had been concluded as depressed meaning comorbid depressive disorder was diagnosed along with Dissociative Fugue.
Interventions
Although there are no evidence-based therapy studies for patients with Dissociative Amnesia, there are three general categories of potential therapeutic approaches: psychopharmacological and somatic treatments, psychotherapeutic interventions, and neuropsychological rehabilitation (Staniloiu & Markowitsch, 2018).
Pyschopharmalogical and Somatic Treatments
Antidepressants have been prescribed to treat cases of Dissociative Amnesia in order to support psychotherapy and improve the mood of the patient. Smith et al. (2010) detailed the case of a patient who experienced functional amnesia after a car accident and could not retain memories from each day after sleeping. She was treated with antidepressants and given encouragement for her memory retention, as well as advised on a regimen that allowed her to sleep for up to four hours nonstop without experiencing memory loss from the previous day’s activities. With this regimen, the patient was able to maintain her memory for successive days two months after she had returned home.
Kosidou & Lindholm (2007) presented the case of a young woman diagnosed with Dissociative Fugue after a history of childhood sexual abuse. She was given a course of electroconvulsive therapy (ECT) and antidepressants, and following the fifth course of ECT she could recall all her past memories. Although ECT has not been proven to be a successful or relevant treatment for Dissociative Amnesia, it has been suggested that it may be essential for easing a comorbid depression.
Although these case studies illustrate possible therapeutic approaches, there is a lack of experimental studies around psychopharmacological and somatic treatment for Dissociative Amnesia. More trials would need to be carried out for the researchers to judge the wider efficacy of these treatments.
Pyschotherapeutic Interventions
Most psychotherapeutic approaches use a plan that begins with an effort to stabilize the personality, since patients with Dissociative Amnesia frequently have a more fragile personality with lower self-esteem, which makes them particularly susceptible to influences from others. The stabilization of the patient’s personality aids in both establishing a psychosomatic model of the patient’s illness and motivating the patient to engage in therapy (Staniloiu & Markowitsch, 2014).
Psychotherapy is the first method of intervention typically chosen due to lack of side effects encountered by a drug-assisted intervention. This is also known as “talk therapy”. In a session, the therapist essentially establishes a sense of security and uses supportive and emotional validation (Bennett, 2019).
In a case analyzed by Dr. Pravesh Sharma et al. (2015), the success of psychotherapy is shown. The patient observed was a 20 year old man who had forgotten his job and had no recollection of people close to him. His mother’s texts and calls were left unanswered and he was perplexed as to why he was in a parking lot when his friends found him. When taken into the inpatient psychiatry unit, his urine drug screen for illicit substances, human immunodeficiency virus, and rapid plasma reagin tests were negative. Complete blood count, complete metabolic profile, ammonia level, B12 level, thyroid function tests, and liver function tests were found to be within normal limits. Any symptoms of depression, anxiety, mania, and/or psychosis were denied, and he had no history of seizure or head trauma. However, no emotional changes were noted from the breakup. The next step was a neurologic workup, including electroencephalogram and brain imaging, in which the organic causes of transient amnesia were ruled out.
Malingering, or faking the illness, was then considered, with a psychology consultation requested. After multiple sessions, the patient began to recall past events including his breakup, which had been painful, and he elaborated by saying he felt numb the day he had begun to forget things. After a set of sessions over the course of 12-16 weeks, he started to remember information about his past. What was found here is the most successful treatment is psychotherapy, creating a safe environment with empathy as opposed to skepticism.
This being one example, there is a lack of sufficient, evidence-based studies analyzing the results of psychotherapy in order to state an effectiveness rate.
Neuropsychological Rehabilitation
Neuropsychological rehabilitation includes individual/group cognitive rehabilitation, psychotherapy, and psychoeducation designed to improve “cognitive, emotional, and psychosocial” functions (Yi, 1970).
There is a shortage of information on the use of neuropsychological rehabilitation as a treatment for Dissociative Amnesia. The majority of the data that is currently available comes from functional amnesia cases, which are defined by a combination of biological (brain damage produced by physical trauma or lesions) and psychological (severe trauma-related stress) factors. They propose that the severe memory impairment brought on by amnesia and quality of life may both be improved by maintaining implicit control of knowledge (Thoene & Glisky, 1995).
In order to maintain safety and monitor the patient, neurorehabilitation treatment must be implemented carefully in coordination with mental health professionals who can assist with moderating emotional reactions.
Conclusion
In conclusion, Dissociative Amnesia has been shown to be an adverse effect that comes from childhood trauma. There are multiple risk factors including age, relationship to abuser, ability to disclose, and head injuries. Additionally, the stimulation of the hippocampus, amygdala, and prefrontal cortex also plays a role in the development of Dissociative Amnesia. Dissociative Amnesia can have detrimental impacts on daily life due to the sudden memory loss, especially in the highlighted case of Dissociative Fugue. It often coexists with other stressors, such as academic pressure or economic strain. Furthermore, there are forms of therapy for Dissociative Amnesia such as psychopharmaceutical and somatic treatments, psychotherapeutic interventions, and neuropsychological rehabilitation.
Unfortunately, Dissociative Amnesia is very difficult to study. As of now, the main evidence comes from case studies, which although they can be very insightful, are often limited to a certain scenario. This means that there are not as many widely generalizable studies and the conclusions reached in these case studies can vary from person to person.
The review of existing evidence around Dissociative Amnesia in scientific literature that has been carried out in this paper has underlined the gap in current evidence-based studies, specifically surrounding Dissociative Amnesia, as many studies include it under an umbrella of ‘PTSD-related disorders’, or solely label it as a constituent of Dissociative Identity Disorder (DID) due to the common comorbidity of these two conditions, when in fact Dissociative Amnesia can occur with an absence of DID.
Although Dissociative Amnesia is still widely unexplored, there is still hope that with the aid of more scientific evidence, one day there will be more available therapies and treatments for this disorder.
Bibliography
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed., text rev.). https://doi.org/10.1176/appi.books.9780890425787
Akirav, I., & Richter-Levin, G. (2006). Factors that determine the non-linear amygdala influence on hippocampus-dependent memory. Dose-response : a publication of International Hormesis Society, 4(1), 22–37. https://doi.org/10.2203/dose-response.004.01.003.Akirav
Alexander, K., Quas, J., Goodman, G., & Ghetti, S. (2005). Traumatic impact predicts long-term memory for child sexual abuse. https://www.researchgate.net/publication/8070317_Traumatic_Impact_Predicts_Long-Term_Memory_for_Documented_Child_Sexual_Abuse
Bennett, C. (2019, February 21). Psychological intervention strategies for dissociative amnesia. News. https://www.news-medical.net/health/Psychological-Intervention-Strategies-for-Dissociative-Amnesia.aspx
Bérubé, A., Turgeon, J., Blais, C., & Fiset, D. (2021). Emotion Recognition in Adults With a History of Childhood Maltreatment: A Systematic Review. Trauma, Violence, & Abuse, 152483802110294. doi: 10.1177/15248380211029403
Bidzan, M. (2017). Biological Bases of Dissociative Amnesia. Acta Neuropsychologica, 15(1), 1-11. doi: 10.5604/12321966.1233199
Brand, M., Eggers, C., Reinhold, N., Fujiwara, E., Kessler, J., Heiss, W., & Markowitsch H. J. (2009) Functional brain imaging in 14 patients with dissociative amnesia reveals right inferolateral prefrontal hypometabolism. Psychiatry Research: Neuroimaging, 174 (1), 32–39.
Clouden, T. A. (2020). Dissociative amnesia and Dissociative Fugue in a 20-year-old woman with schizoaffective disorder and post-traumatic stress disorder. Cureus. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7255065/
Cuncic, A. (2020). What is Dissociative Fugue? Verywell Mind. https://www.verywellmind.com/an-overview-of-dissociative-fugue-4770158
Dimitrova, L., Dean, S., Schlumpf, Y., Vissia, E., Nijenhuis, E., & Chatzi, V. et al. (2021). A neurostructural biomarker of dissociative amnesia: a hippocampal study in dissociative identity disorder. Psychological Medicine, 1-9. doi: 10.1017/s0033291721002154
DoveMed. (2020). Dissociative Amnesia. https://www.dovemed.com/diseases-conditions/dissociative-amnesia/
Duggal, S., & Sroufe, L. A. (1998). Recovered memory of childhood sexual trauma: A documented case from a longitudinal study. https://www.researchgate.net/publication/13714385_Recovered_memory_of_childhood_sexual_trauma_A_documented_case_from_a_longitudinal_study
Freyd, J.J. (2013). What is a betrayal trauma? What is betrayal trauma theory? https://scholarsbank.uoregon.edu/xmlui/bitstream/handle/1794/65/defineBT.html?sequen
Hannibal, K., & Bishop, M. (2014). Chronic Stress, Cortisol Dysfunction, and Pain: A Psychoneuroendocrine Rationale for Stress Management in Pain Rehabilitation. Physical Therapy, 94(12), 1816-1825. doi: 10.2522/ptj.20130597
Igwe, M. N. (2013). Dissociative fugue symptoms in a 28-year-old male Nigerian Medical Student: A case report – journal of medical case reports. BioMed Central. Retrieved August 18, 2022, from https://jmedicalcasereports.biomedcentral.com/articles/10.1186/1752-1947-7-143
Joseph, R. (1999). The neurology of traumatic “dissociative” amnesia: commentary and literature review. Child Abuse & Neglect, 23(8), 715-727. doi: 10.1016/s0145-2134(99)00048-4
Kosidou, K., & Lindholm, S. (2007). A rare case of dissociative fugue with unusually prolonged amnesia successfully resolved by ECT. European Psychiatry, 22, S264-S265. doi: 10.1016/j.eurpsy.2007.01.889
McEwen, B. (1993). Stress and the Individual. Archives Of Internal Medicine, 153(18), 2093. doi: 10.1001/archinte.1993.00410180039004
Melchert, T. P., & Parker, R. L. (1997). Different forms of childhood abuse and memory. https://www.ojp.gov/ncjrs/virtual-library/abstracts/different-forms-childhood-abuse-and-memory
Nejad, A. G., & Farahati, H. (2007). Dissociative Disorders and dissociative symptoms among veterans of the Iraq-Iran War suffering from chronic post-traumatic disorder. Neurosciences Journal. Retrieved August 20, 2022, from https://nsj.org.sa/content/12/4/318.abstract
Odagaki, Y. (2017). A case of persistent generalized retrograde autobiographical amnesia subsequent to the Great East Japan earthquake in 2011. Case reports in psychiatry. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5350489/
Phelps, E., & LeDoux, J. (2005). Contributions of the Amygdala to Emotion Processing: From Animal Models to Human Behavior. Neuron, 48(2), 175-187. doi: 10.1016/j.neuron.2005.09.025
Poljac, E., Montagne, B., & de Haan, E.H. (2011) Reduced recognition of fear and sadness in posttraumatic stress disorder. Cortex, 2011, 47 (8), 974–980.
Rauch, S., Whalen, P., Shin, L., McInerney, S., Macklin, M., & Lasko, N. et al. (2000). Exaggerated amygdala response to masked facial stimuli in posttraumatic stress disorder: a functional MRI study. Biological Psychiatry, 47(9), 769-776. doi: 10.1016/s0006-3223(00)00828-3
Sharma, P., Guirguis, M., Nelson, J., & McMahon, T. (2015, May 28). A case of dissociative amnesia with dissociative fugue and treatment with psychotherapy. The primary care companion for CNS disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4578902/
Smith, C., Frascino, J., Kripke, D., McHugh, P., Treisman, G., & Squire, L. (2010). Losing memories overnight: A unique form of human amnesia. Neuropsychologia, 48(10), 2833-2840. doi: 10.1016/j.neuropsychologia.2010.05.025
Staniloiu, A., & Markowitsch, H. (2014). Dissociative amnesia. The Lancet Psychiatry, 1(3), 226-241. doi: 10.1016/s2215-0366(14)70279-2
Staniloiu, A., & Markowitsch, H. (2018). Dissociative Amnesia – A Challenge to Therapy. International Journal Of Psychotherapy Practice And Research, 34-47. doi: 10.14302/issn.2574-612x.ijpr-18-2246
Thoene, A. I., & Glisky, E. L. (1995). Learning of name–face associations in memory impaired patients: A comparison of different training procedures. Journal of the International Neuropsychological Society, 1(1), 29-38.
Wolf, M. R., & Nochajski, T. H. (2013). Child sexual abuse survivors with dissociative amensia: What’s the difference? Journal of Child Sexual Abuse, (May). https://www.researchgate.net/publication/236851529_Child_Sexual_Abuse_Survivors_with_Dissociative\_Amnesia_What’s_the_Difference_Journal_of_Child_Sexual_Abuse_224_462-480
Yi, A., & Belkonen, S. (1970). Neuropsychological rehabilitation. SpringerLink. https://link.springer.com/referenceworkentry/10.1007/978-0-387-79948-3_1096